Varicose Veins / Chronic Venous Insufficiency: Evaluation and New Treatment Options
by: Susan B. Fox, D.O, RPVI, FSVM
In the United States, venous disease is very prevalent and in one US health survey, varicose veins were found to be the 7th most common reason for medical referral. Venous disease is a spectrum of disease that ranges from spider veins to increasing degrees of venous insufficiency. Approximately, 25% of all women and 15% of all men have some degree of venous insufficiency. As one ages this increases and after age sixty, 72% of all women and 40% of all men are affected by venous insufficiency.1 Sapheno-femoral incompetence causing reflux in the greater saphenous vein (GSV) is the most common cause of venous insufficiency in symptomatic patients. This reflux often results in multiple varicosities of the lower extremity. If this reflux is not treated approximately 50% of patients will develop venous hypertension with symptoms of chronic venous insufficiency.2 With progressive degrees of reflux patients develop increasing symptoms of leg pain, swelling, venous hemorrhage, venous eczema, lipodermatosclerosis and in some cases even venous ulcerations. Venous stasis ulcers are the most common cause of lower extremity ulceration. Greater than 1 million Americans have  and greater than 100,000 people are totally disabled from them. Venous stasis ulcers are a huge burden on the US health care system, costing on average 2.5 to 3 billon dollars/year (> 2% of the national health care budget) and between 3 and 4 million lost workdays each year. 3,4 It is important to notice venous insufficiency early in its course and treat appropriately before the patient develops one of these ulcers.
and greater than 100,000 people are totally disabled from them. Venous stasis ulcers are a huge burden on the US health care system, costing on average 2.5 to 3 billon dollars/year (> 2% of the national health care budget) and between 3 and 4 million lost workdays each year. 3,4 It is important to notice venous insufficiency early in its course and treat appropriately before the patient develops one of these ulcers.
Patients with mild to moderate disease will complain of restless leg syndrome, night cramps, heavy or tired legs at the end of the day, or a burning or aching feeling in the leg. With increasing disease, they will often have symptoms of increasing leg pain, edema, venous hemorrhage, superficial or deep vein phlebitis, PE, or leg ulcers. Small telangiectasias cause symptoms in about 53% of patients. 5 Whereas increasing degrees of venous insufficiency will cause symptoms in an increasing number of patients. With the increasing insufficiency patients also develop increasing degrees of venous tissue damage. They will have more chronic stasis changes on examination such as melanin deposition, lipodermatosclerosis, stasis dermatitis, atrophie Blanche, edema and
ulcerations.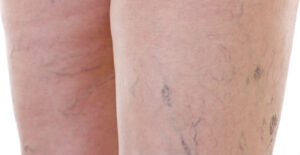
How to diagnose venous insufficiency:
Since venous insufficiency is so prevalent, it is important to notice the signs and symptoms in your patients. A good history and physical exam are vital. Ask patients if they have any symptoms and look for varicose veins, leg swelling, melanin deposition around their ankles. With increasing degrees of insufficiency, patients will have increasing degrees of venous tissue damage. They will have more chronic stasis changes on examination such as venous eczema, increased areas of melanin deposition, lipodermatosclerosis, stasis dermatitis, atrophie blanche, edema and ulcerations
.
These people should be checked for concomitant arterial disease. They should have their pedal pulses evaluated. There are many clinical diagnostic tests that can be used to diagnose venous reflux. However, these tests are relatively insensitive and the “gold standard” test is a Doppler ultrasound. A valvular incompetency study should be performed. It will tell if there is a phlebitis if there is reflux in the deep or superficial venous system and may reveal incompetent perforator veins. This test needs to be performed by a trained vascular technologist to be done properly.
Conservative treatment:
If the pulses are normal, the patient should be prescribed a trial of graduated compression hose. These should not be over the counter support stockings but rather prescription-strength compression hose that should be worn daily. They should wear them from the minute that they get out of bed until they lie down to sleep. Patients should be encouraged to elevate their legs. If there are no contraindications, they may sleep with the foot of their bed elevated 4 to 6 inches to reduce swelling. As well, they should moisturize their legs daily to help prevent any skin breakdown and ulcer development. Good foot care is a must and will help prevent the development of cellulitis. We are the best vein doctor in Miami.
The narrowest part of the ankles and widest part of the calves should be measured when their swelling has diminished and / or first thing in the morning when their legs are the thinnest to ensure that the hose is fit properly. If patients are very obese or have heavy legs they may require custom-made stockings. Patients should be educated on how to wear and care for the hose. (They should be instructed not to roll over the top of the hose. For knee -highs they should not be pulled up any higher than 2 fingers below their knees. They should not be put in the drier. To help put on the hose the patients should wear gloves and put them on dry skin. They can purchase a stocking donner if they have difficulty pulling on the hose or have weak hands.)
There are multiple herbal medications that may help with venous insufficiency Bilberry fruit extract (Vaccinium myrtillus) 80 to 160 mg tid, Horse chestnut seed extract (Aesculus hippocastanum) 300mg twice daily and Pycnogenol (Pinus Maritima) 100mg tid. Studies have shown decreased edema with each of these. There were no side effects reported with any of these medications but the long- term, well-controlled trials are lacking.6 As well, there are mediations not available in the US called micronized flavonoids such as Daflon 500mg that decrease the symptoms of venous disease and decrease leg edema. These medications are helpful in patients who cannot tolerate compression bandages or as an adjunct to the bandages.
Definitive Treatment:
Conventional therapy for venous insufficiency is ligation of the saphenofemoral junction with or without stripping of the varicosities. Although this technique has been used by vascular surgeons for years, postoperative morbidity is high. The most common complications are with general anesthesia. There is a great deal of post-operative pain, a high number of saphenous nerve injuries or irritation, infections, neovascularization, hematomas and DVT’s. High ligation plus vein stripping has an 86% immediate success rate but patient satisfaction with the procedure was only about 62%.7 It seems that even when the surgery is performed correctly there is a high recurrence of varicose veins after vein ligation and stripping. This is felt to be due to neovascular (new vessel formation) reconnection and persistent abnormal venous physiology. In one study, neovascularization was present in 52.7% of patients after vein stripping and ligation. 8 Several studies have shown high recurrence rates after vein ligation with or without vein stripping. In a study done to assess the recurrence rate of varicosities after vein surgery, there was a 47% rate of recurrence at 3 years and 66% at 5 years.9 In recent years new, minimally invasive vein treatment options have become available. Our practice in Miami foam sclerotherapy (not FDA approved in the United States), VNUS closure and endolaser vein ablation.
Foam sclerotherapy has been used in Europe for several decades. This technique is not FDA approved in the US. There are multiple different techniques that have been invented to create a foam out of various strengths 2 detergent based sclerosants which are not FDA approved in the US. By mixing the solution with air or CO2, a foam is formed. The foam totally fills the vessel, displacing blood thus having greater contact with the vein lining. The benefit over conventional sclerotherapy is that the foam stays in contact with the vein lining for a greater period of time causing more irritation. Sclerotherapy is not conventionally used to treat veins over 6mm due to a high degree of recurrence. However, with foam the results are much better. In one study, 92% of visible varicose veins were successfully treated and the other 8% showed improvement. 10 In another study treating the greater saphenous vein, 80% of the veins treated disappeared totally with a recurrence of 15% at 2 years.11 Due to the fact that there are various methods of creating foam, there are no good prospective randomized trials. Side effects include chest pain, TIA’s/ scotomas, visual disturbances such as blurring, monocular blindness lasting a few hours, vomiting, phlebitis, an impression of “bad taste”, staining, skin necrosis, shortness of breath and migraines. These have been found to be only transient to date. There is also a risk of DVT or PE (non documented in the literature) as with any venous treatment modality. It is proposed that it would take 480cc introduced over 20 to 30 seconds in a 60kg man to kill him. 12 However, it is estimated that as little as 150 cc of air injected could kill a human.
Know about the Treatment of Vein Disease
VNUS was approved in Europe in 1998 and the US in 1999. VNUS closure involves placing a radio frequency catheter into the vein being treated and sealing it shut from the inside. A radio frequency catheter is threaded into the vein under ultrasound guidance and plugged into a machine that heats the probes up to 85 degrees C. The catheter is pulled back very slowly and causes scarring of the vein lining, sealing it shut. The procedure can be performed for veins 2 to 12 mm. One of the drawbacks of this technique is that there is a 12 mm size limit on the size of the veins that can be treated due to the catheter limitations. Physicians can get around this to some degree by compressing the vein with tumescent anesthesia (a large amount of anesthetic solution injected into the tissue) or by injecting a sclerosing solution or foam into the vein once the radio frequency probe is inside to spasm the vein down around the catheter. However, most insurance agencies will not cover treatment of a vein greater than 12mm in diameter. The procedure has an immediate success rate of 92.7 to 98% and a 10% recurrence rate at 1 and 2 years. 13,14,15,16. However, in several of the studies the patients had also undergone high ligation of the GSV, as well. Two other studies reported acute success rates of closure to be only 68 and 73%. 17,18 The procedure can be done under local anesthesia. However, frequently it is done in the operating room under general anesthesia. The drawbacks are that it has a size limit to the veins that can be treated, neovascularization, potential nerve damage, skin paresthesias, skin burns, DVT or PE, edema, hematoma, ecchymosis, transient pain and tenderness. The length of recovery is very short and most people are back to work and their regular activities within a few days. The average time off work was 6.5 days with VNUS and 15.6 days with stripping.
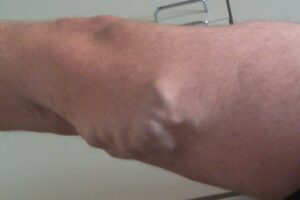 Endovenous laser ablation of the varicose veins is the newest and least invasive technique to treat GSV reflux. It was FDA approved in the US in January of 2002. The procedure can be performed in an outpatient office or procedure room. A modified Seldinger technique is used under ultrasound guidance to gain access to the GSV. The laser is threaded into the vein. The entire procedure takes on average, 45 minutes. A bandage and compression hose 30to 40 mm/hg is applied. The patient is encouraged to walk for 30 to 45 minutes, daily starting immediately after the procedure. They return for a follow-up ultrasound between 4 and 7 days post operatively to ensure closure of the GSV and patency of the common femoral vein. There have been very few side effects in the studies to date. Minor complications include mild non-entry site bruising and a delayed pulling sensation (described as a mild sore muscle sensation) along the course of the GSV that peaks at around 4 to 7 days post- treatment. Other side effects have been very infrequent in the literature and include minor skin burns, hematomas, infections, paresthesias and DVT. The benefits are that the procedure is done solely under local anesthesia, thus avoiding the risks associated with general anesthesia, the procedure is faster and easier to do, the patient is ambulatory immediately following the procedure and because recovery time is only a few days people can return to work almost immediately. There have been several clinical reports from 2001 to 2004 that document an acute success rate of 90.4 to 100% with a 2 year recurrence at <4%.20,21,22,23. In a survey of patients following the procedure 99.8% of patients said that were satisfied with treatment and would refer a friend for the procedure.24
Endovenous laser ablation of the varicose veins is the newest and least invasive technique to treat GSV reflux. It was FDA approved in the US in January of 2002. The procedure can be performed in an outpatient office or procedure room. A modified Seldinger technique is used under ultrasound guidance to gain access to the GSV. The laser is threaded into the vein. The entire procedure takes on average, 45 minutes. A bandage and compression hose 30to 40 mm/hg is applied. The patient is encouraged to walk for 30 to 45 minutes, daily starting immediately after the procedure. They return for a follow-up ultrasound between 4 and 7 days post operatively to ensure closure of the GSV and patency of the common femoral vein. There have been very few side effects in the studies to date. Minor complications include mild non-entry site bruising and a delayed pulling sensation (described as a mild sore muscle sensation) along the course of the GSV that peaks at around 4 to 7 days post- treatment. Other side effects have been very infrequent in the literature and include minor skin burns, hematomas, infections, paresthesias and DVT. The benefits are that the procedure is done solely under local anesthesia, thus avoiding the risks associated with general anesthesia, the procedure is faster and easier to do, the patient is ambulatory immediately following the procedure and because recovery time is only a few days people can return to work almost immediately. There have been several clinical reports from 2001 to 2004 that document an acute success rate of 90.4 to 100% with a 2 year recurrence at <4%.20,21,22,23. In a survey of patients following the procedure 99.8% of patients said that were satisfied with treatment and would refer a friend for the procedure.24
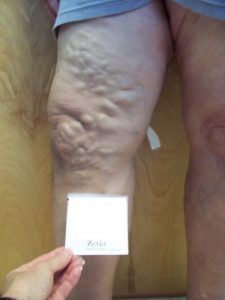
SP pre endovenous laser
The Clarivein procedure is the newest FDA approved procedure that is performed for varicose veins. It is another minimally invasive procedure used to close saphenous veins or their tributaries in patients with venous insufficiency or varicose veins. The Clarivein procedure normally uses only one injection of local anesthetic and usually can be performed without any incisions. The Clarivein procedure is done in the office in minutes. The physician numbs one spot on the skin and places a wire that rotates inside the incompetent vein. The wire rotates while a detergent based sclerosant is injected into the vein. The patient receives only one or two injections of local anesthetic and can return to their normal activities immediately. The average treatment takes less than 5 minutes and the whole procedure is performed in less than 15 minutes. It has a success rate of 99%.
Fort Lauderdale vein Doctor Susan B Fox DO, RPVI, FSVM is board certified in the treatment of veins and in vascular medicine. She completed her residency and vascular fellowship in the Cleveland Clinic in Cleveland, Ohio Dr Susan Fox specializes in the non-surgical treatment of varicose and treatment of spider veins using state of the art minimally invasive therapy. She has successfully treated tens of thousands of veins and serves as a training facility for venous techniques. She sees patients in Miami, Hollywood, and Pembroke Pines. Dr. Fox has been featured on several
Read more Blogs:


